Key Takeaways
- Bunions are often hereditary and can become more severe if left untreated.
- Conservative measures only relieve symptoms and cannot correct the underlying bone deformity.
- There are different surgical procedures, so your recovery will vary depending on your specific case.
- Working with a qualified foot and ankle surgeon is important for personalized recommendations and better outcomes.
Table of Contents
- What Are Bunions?
- Are Bunions Hereditary?
- Do Over-the-Counter Pads and Splints Work?
- Will My Bunion Get Worse?
- When Should I Consider Surgery?
- What Does Bunion Surgery Involve?
- How Long Is the Recovery Period?
- Can Bunions Recur After Surgery?
Bunions can disrupt your daily life, causing discomfort and limiting the type of shoes you can comfortably wear. If you are struggling with persistent bunion pain, you might be considering your options and wondering where to turn for the best care. Thankfully, speaking with a bunion surgeon near me can help clarify whether surgery is right for you and answer any pressing questions about your situation and options.
Getting informed about the causes, symptoms, and treatments of bunions puts you in a better position to make decisions about your foot health. While many worry about the prospect of surgery, understanding what to expect and reviewing commonly asked questions can ease your mind. This article aims to empower you with accurate, useful information so you can take the next step confidently if you need intervention for bunion pain.
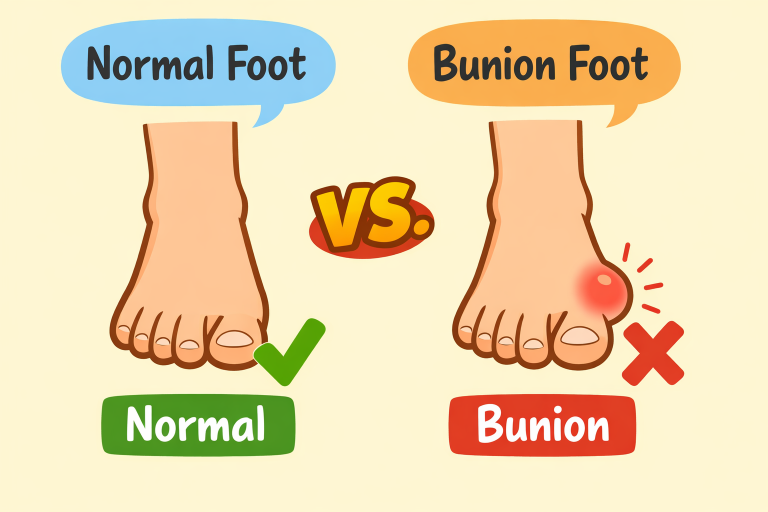
What Are Bunions?
A bunion, or hallux valgus, is a bony protrusion that develops at the joint located at the base of your big toe. This bump forms when the bones in the front part of the foot become misaligned. As a result, the big toe is pushed toward the second toe, which can cause significant discomfort, inflammation, and challenges in finding properly fitting footwear.
Are Bunions Hereditary?
Research demonstrates that bunions are often linked to genetic factors. While the bunion itself is not directly inherited, the foot shape and structural tendencies that increase bunion risk can be passed from parents to children. If your mother, father, or close relatives have had bunions, you may be at higher risk of developing them as well. Other contributing factors can include unsupportive shoes, arthritis, and certain neuromuscular conditions.
Do Over-the-Counter Pads and Splints Work?
Products like bunion pads, gel cushions, and splints can reduce some symptoms associated with bunions, including friction- or pressure-related pain. However, it is important to understand that these options act as temporary solutions. They do not address the underlying bone alignment problem or permanently alter the course of the condition. Relying solely on padding and splints may offer comfort but will not reverse or stop bunion progression.
Will My Bunion Get Worse?
Bunions are considered a progressive condition. In most cases, the bump, pain, and discomfort increase over time, especially when left unmanaged. The progression can be influenced by factors such as continued pressure from tight shoes, high heels, or prolonged standing. While some people may have slow progression, others may notice symptoms worsening more rapidly. Early intervention can help slow progression and better manage symptoms. For a comprehensive guide on bunions, visit the Mayo Clinic’s page on bunions.
When Should I Consider Surgery?
If conservative treatments like wider shoes, over-the-counter pain relief, or custom orthotics are not controlling your pain or the bunion is interfering with usual activities, surgery may be appropriate. Surgery is generally recommended only when pain is significant and all other methods have failed, rather than for cosmetic reasons. Your foot and ankle surgeon can review your medical history, lifestyle needs, and x-rays to advise on the right timing and approach for you. Consulting a specialist helps ensure the best possible outcomes, as seen in recommendations by Harvard Health.
What Does Bunion Surgery Involve?
Bunion surgery is called a bunionectomy and involves removing the swollen tissue, correcting the alignment of the big toe by repositioning bones and tendons, and often shaving down the bony bump. More than 100 different bunion surgery techniques exist, so the specific method used will depend on the severity of your bunion and the surgeon’s evaluation. Some procedures are minimally invasive and require only small incisions, while others involve more extensive restructuring and bone work for severe deformities. Your surgeon will review risks, anesthesia options, and what to expect during and after the procedure.
How Long Is the Recovery Period?
Recovery time after bunion surgery depends largely on the type of procedure performed. Less invasive surgeries can allow partial weight-bearing within a few days or weeks, while more complex corrections may require several weeks of non-weight-bearing and up to 6 months for a full recovery. Most people require special footwear or crutches in the early stages of healing. Swelling and mild discomfort may persist for months, and following your surgeon’s recovery instructions is crucial for the best outcome.
Can Bunions Recur After Surgery?
While bunion surgery aims to correct the deformity and relieve pain, there is always a risk that bunions can recur, especially if contributing factors are not addressed after healing. Wearing shoes with good support, using orthotic devices if recommended, maintaining a healthy weight, and performing foot exercises can decrease the chances of recurrence. Making thoughtful choices about footwear and foot health after surgery is essential for maintaining your results long term.
For more thorough information on bunion treatment and surgery options, trusted resources such as the American College of Foot and Ankle Surgeons provide reliable education and advice.
Always consult a trained healthcare professional or foot specialist for individualized care and recommendations based on your specific situation. They will guide you through diagnosis, treatment planning, and follow-up to help you achieve the best possible results for your foot health.